Physician Compensation Review is a Strategic Opportunity
Your work has value. Your compensation methodology should reflect it.
Spring 2026 By Jessica Minesinger, CMOM, CMPE, FACMPE, BBCC
Physician compensation methodology is not “just a formula.” It reflects how an organization values physician expertise, access, productivity, quality, leadership, and the realities of clinical practice.
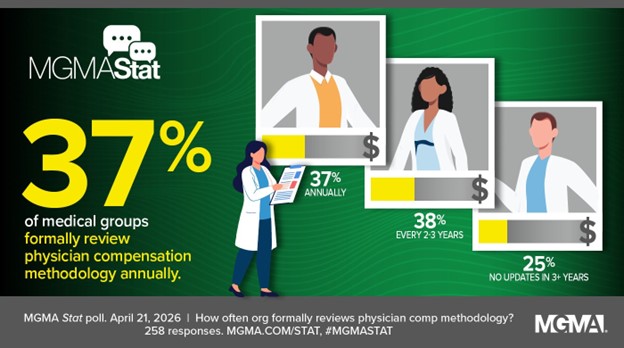
A recent MGMA Stat article, “Falling behind on physician compensation plan review carries real risk,” notes that most medical groups formally review their physician compensation methodology annually or every 2 to 3 years. However, one in four medical groups has not updated its approach in the past 3 years. The article also emphasizes that compensation methodology directly affects recruitment, retention, regulatory compliance, and organizational culture.
For physicians, this matters.
Compensation models often include more than base salary and productivity. Depending on specialty and practice setting, they may incorporate quality metrics, patient access, panel size, APP supervision, administrative duties, medical directorships, call coverage, care coordination, and other responsibilities that support patient care and organizational performance.
MGMA also highlights a major 2026 issue: CMS’s new efficiency adjustment reduces work RVUs for most non-time-based services by 2.5%. Physicians may perform the same work but generate fewer wRVUs because CMS changed the measurement—not because their effort, productivity, access, or value declined.
That distinction is critical.
For physicians and medical groups, compensation review should be proactive, not reactive. It is an opportunity to evaluate whether thresholds, conversion factors, bonus structures, quality incentives, leadership stipends, and productivity expectations remain aligned with current market data and actual physician work.
Special Compensation Consideration for Surgeons
For surgeons, compensation review deserves additional attention. Surgical compensation may be influenced by OR access, procedural volume, case complexity, trauma or emergency call, inpatient coverage, perioperative leadership, APP supervision, service-line growth, and the resources required to sustain a surgical program.
A surgical compensation model that focuses solely on wRVUs doesn’t reflect contributions essential to access, program stability, and quality patient care. This is especially important when CMS valuation changes may reduce wRVU credit for the same clinical work.
A strong physician compensation review should ask:
- Are benchmarks current, specialty-specific, and regionally relevant?
- Has the organization modeled the 2026 wRVU impact by specialty and CPT code mix?
- Are access, quality, call, APP supervision, administrative work, on-call expectations, and leadership appropriately valued?
- Is the methodology understandable, transparent, and defensible?
- Does the model support recruitment, retention, physician engagement, and long-term practice strength?
Bottom line: Your work has value. As a physician, compensation review is not just about identifying what needs to change—it is an opportunity to create clarity, strengthen trust, and ensure your compensation methodology reflects the care you provide, the responsibilities you carry, and the value you bring—with fairness, transparency, and a plan for the future!
Work With SCC to Strengthen Your Compensation Strategy
Customized Compensation Consulting for Physicians
At SCC, we are Physician Advocates! We specialize in this important work, helping physicians navigate compensation opportunities and verify fair pay. We would be delighted to work with you to provide data-driven guidance as you navigate your professional journey.
Connect with us for one-on-one coaching support focused on physician compensation and negotiation. We can review your current compensation, analyze it using MGMA Physician Compensation Data and benchmarks, offer negotiation recommendations, and create a customized consultation plan tailored to your goals.